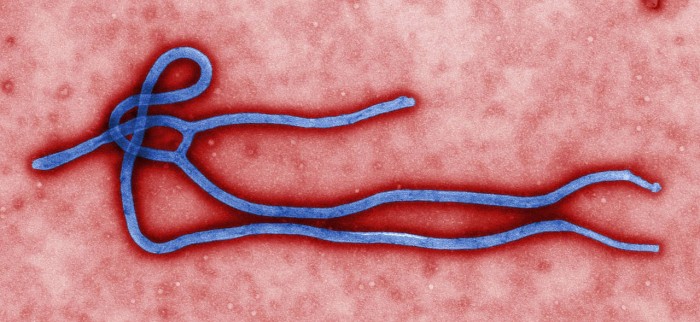
Ebola has been making lots of news this year, as the virus has popped up in several West African countries. We are in the midst of the largest and most widespread outbreak in history.
Fruit bats are the main carriers of the virus in nature. Initially, humans become infected with the ebola virus after contact with infected bats or any living or dead animals that have been infected by the bats. This contact is often thought to be from consumption of infected meat. After humans become infected, the disease spreads through contact with infected bodily fluids including sweat, saliva, urine and semen. Ebola is insidious, and in some cases can take up to 21 days after exposure before symptoms manifest. Symptoms include a sudden onset of flu-like fever, ache and fatigue followed by vomiting or diarrhea.
Sky News details why the virus is so deadly:
When ebola enters the body, it targets dendritic cells in the immune system. Normally, when a virus is detected, these cells tell other cells to produce antibodies. Ebola prevents that signal getting out. As far as the immune system knows, everything inside the body is fine. Left alone, ebola then begins replicating rapidly. It then spreads into the bloodstream, infecting the whole body. Cells start to break up and die, in huge numbers. That finally triggers the immune system, which kicks in – far too aggressively.
Ordinarily when you get sick, the body releases proteins called cytokines. Some of these cells tell your blood vessels to become more permeable. This is to let antibodies travel through the body more quickly to fight the disease. But once ebola has taken hold of your body, the immune system reacts much too aggressively – and launches a cytokine storm. This causes blood vessels to become far too permeable, and they leak. At the same time, the body’s blood clotting mechanisms also act abnormally. This causes internal and external bleeding and is why ebola is known as a haemorrhagic fever. It causes tissue damage and organ failure.
Though the disease is deadly, people do survive and countries can contain outbreaks. Survivors’ blood may contain antibodies that can be used to treat others suffering from the disease.